Expanding contact tracing and testing to anyone exposed to Covid-19, including those who were asymptomatic, may have enabled the San Francisco Department of Public Health to diagnose more Covid-19 patients, according to a research letter published by the Journal of the American Medical Association on Monday.
The research letter and data analysis was led by the Health Department and University of California San Francisco doctors, and evaluates contact tracing data from April 13 to June 8, 2020. In April, the Health Department followed Centers for Disease Control and Prevention’s recommendation to test only symptomatic close contacts of infected people; that changed May 5, according to the research letter.
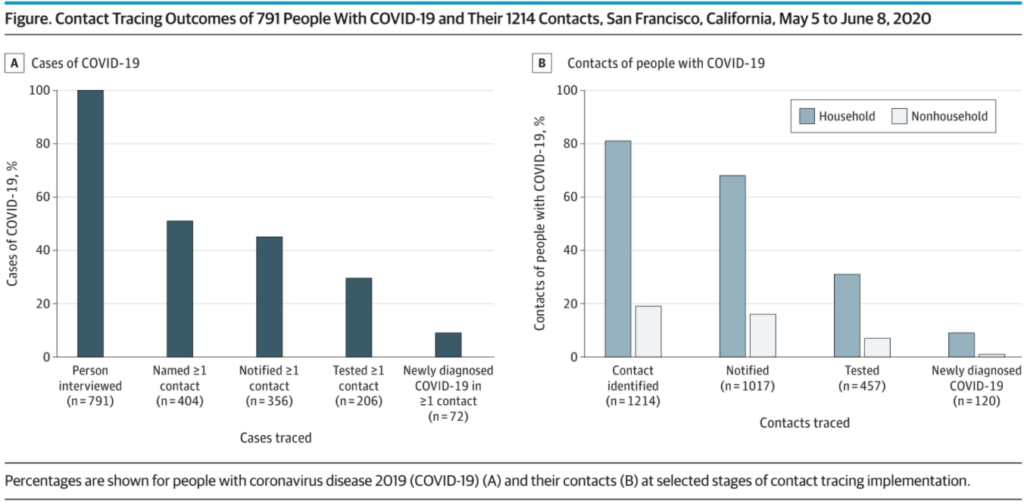
Since the shift in strategy, the letter’s data showed 37 percent of people who were exposed by infected San Franciscans got contacted and tested, and 10 percent of them were newly diagnosed with covid in a time when the citywide covid positivity rate was 2.2 percent.
“Through these efforts, we were able to identify many people who otherwise would not have known about their Covid-19 diagnosis,” said Dr. Darpun Sachdev, the Health Department’s lead expert on covid contact tracing. “It’s absolutely essential that we reach out and offer testing and supportive services to all contacts.”
Numerous medical experts have said that case investigation and contact tracing can be key strategies to limiting the spread of the virus and combating the pandemic. Case investigation is when an infected person is interviewed about symptoms and who they came in contact with, and are offered access to services. Contact tracing is when close contacts of infected people are identified, called and encouraged to get tested.
Contact tracing can be helpful if enough people are reached quickly and if close contacts actually get tested and quarantine. Medical experts have said covid-positive patients are most infectious when symptoms first appear, and up to five days after. That means accelerating the process of diagnosis to isolation can significantly curb transmission.
Since the research letter’s data collection, the Health Department has sped up its ability to identify secondary cases, or a close contact of someone who also got sick. In the spring, contact tracers identified secondary cases within a median of six days from symptom onset. Now it is down to five, Sachdev said.
This delay “raises concern regarding the timelines of tracing in preventing onward transmission,” the letter stated. Currently, case investigation and contact tracing begins the same day someone is diagnosed, in comparison to one day for each in the spring, Sachdev said.
“Our contact tracing team prioritizes people who are contacts by offering them testing through our city test sites, as well as through our other sponsored sites, so we can get same day or next day testing for all of our contacts,” Sachdev said.
But the Health Department has yet to realize their goal of reaching 90 percent of contacts and to investigate 90 percent of cases. Right now, the Health Department is investigating 84 percent of cases, and about 86 percent of the infected individual’s contacts are being reached. Even with fewer people contracting the virus lately, higher outreach to cases and contacts have not substantially increased since the beginning of the crisis.
And the number of people who actually got tested after receiving an exposure notification is even lower, though it has improved, Sachdev said. As of September, 59.6 percent of people who learned they were exposed got tested, compared to the 37 percent who did back during the spring research. Out of the 704 Latinx residents notified in September, 56.4 percent of them tested.
One of the biggest obstacles to reaching more people is whether or not they answer the call in a timely manner, if at all, said Veronica Vien, the public information officer at the Health Department.
“We need folks to help us, and we need them to pick up,” Vien said.
Sachdev said the Health Department calls people several hours for consecutive days. If they still don’t answer, the department texts them or mails them a packet of coronavirus information and Health Department information.
Contact tracing and case investigation are just one indicator in the city’s reopening strategy and for combatting the pandemic, Vien said. The other indicators are testing, access to personal protective equipment, hospitalization availability, and case rates.
“When we are using [contact tracing] as one of the factors among all five, it kind of changes the context a little bit,” Vien said.
On the other front, case investigation among the Latinx population has made gains. The research letter said of the 1,394 people that were successfully interviewed after contracting covid back in the spring, nearly 70 percent identified as Latinx, which may suggest case investigators are reaching the right people. Latinx residents have consistently made up nearly 50 percent of all San Francisco cases, even though they comprise only 15 percent of the population.
By Sept. 11, Sachdev said she estimated that about 90 percent of Latinx cases were investigated, a 20 percent increase that meets the case investigation goal.
The doctor attributes that to two main factors: ramped up testing by the Health Department this summer, and an emphasis on hiring bilingual contact tracers and case investigators. Community groups have also been educating and encouraging locals to get tested, especially at low-barrier neighborhood pop-ups.
“We’ve been focusing on ensuring that we now stratify our outcomes by race, recognizing just how important that is,” Sachdev said.
As of Sept. 25, the department has 146 contact tracers, 43 percent which are bilingual. Of total bilingual contact tracers, 60 percent speak Spanish. Out of the 80 case investigators, 76 percent are bilingual employees, and 62 percent of those speak Spanish.
And, the data underscored a theory that low-income Latinx families who live in overcrowded spaces may have a higher chance of contracting the virus. Researchers found it was more likely that someone who was exposed to a person with covid also got sick — otherwise known as a secondary case — if they lived in the same household. Ninety percent of the secondary cases lived in the same household, according to the data.
The research showed that out of everyone who was interviewed, about 43 percent of respondents lived in a household with five or more people, and about 84 percent of those identified as Latinx.
As the pandemic persists, Sachdev said it remains a priority to find new strategies to improve the program.
“It’s all about looking at our data and trying to identify new ways of doing the work,” Sachdev said. “Just paying close attention to how we can constantly optimize.”
We explain the news. We find out what happens behind the scenes. Support our work here.


Contact tracers should not just be “calling,” “texting,” and “mailing.” They should be banging on peoples’ doors, with testing materials in hand.