Good morning, Mission, and welcome to Virus Village, your (somewhat regular) Covid-19 data dump.
Hospitalizations remain flat, recorded infections take a dip, but positivity rates keep rising, R Number models are back up and wastewater monitoring (at Southeast San Francisco) is trending downward off its recent peak, but still indicating much higher levels of community spread than recorded infections are.
This week it’s all about BA.5, the current leading “variant of concern” that’s ripping through California and the country, causing, or contributing to, a steady stream of infections and hospitalizations. It’s a surge unlike those of the past. What does it mean?
For one, a lot more infections. Here is a sequel to a piece by Eric Topol that Covid Tracker linked to last week. And here is a take from Nature.
Here’s the official version (get boosted).
And don’t miss the U.S. Centers for Disease Control and Prevention’s version of the bumbling Inspector Clouseau from the old Pink Panther movies. Under former President Donald Trump, the CDC revealed a stunning lack of data collection and analysis. Now, over a year into a new administration, not much has changed.
Ed Yong in The Atlantic provides the question posed by BA.5: Should we still care about preventing infection?
San Francisco’s intrepid Department of Public Health won’t answer Yong’s question directly (nothing quite as comforting as opacity from public health officials during a pandemic), but apparently the DPH has moved on to monkeypox.
And, don’t look now, but a new, possibly more dangerous, variant has shown up in India.
My favorite vaccine optimist has more encouraging news on the vaccine front. The Moderna “bivalent” candidate for the next booster has been shown to produce more protection from BA. 5. However, it’s unclear how long those protections will last.
Last month, Chinese scientists concluded a study during the omicron outbreak describing the spectrum of clinical features, risk factors for progression, and dynamic changes in viral load among initially non-severe omicron-infected patients.
In the study cohort of 33,816 diagnosed with non-severe Covid-19 infections upon hospital admission, 22 patients developed severe/critical infections. All were in the risk group of patients over 60, who had stable underlying medical conditions.
Studies to estimate the magnitude of asymptomatic covid cases have found the proportion of asymptomatic covid ranges widely, from 1.4 percent to 78.3 percent. A new study estimates the asymptomatic proportion on the low end. Testing in China, on the other hand, shows asymptomatics at the high end.
While much gets made of China’s “draconian” policies, little or nothing gets reported on what happens to those who question the official line in other countries. Consider the case of David Berger, who criticized Australia’s recent surrender to the virus on the transmission front.
Finally, there is little understanding of how covid gets transmitted, or not, through close contact. Studies have shown the frequency of secondary attack rates varied between 2.1 percent and 75 percent. Like in almost every area of covid data collection and reporting, there are no standardized guidelines for reporting transmission in close contact settings
Scroll down for today’s covid numbers.
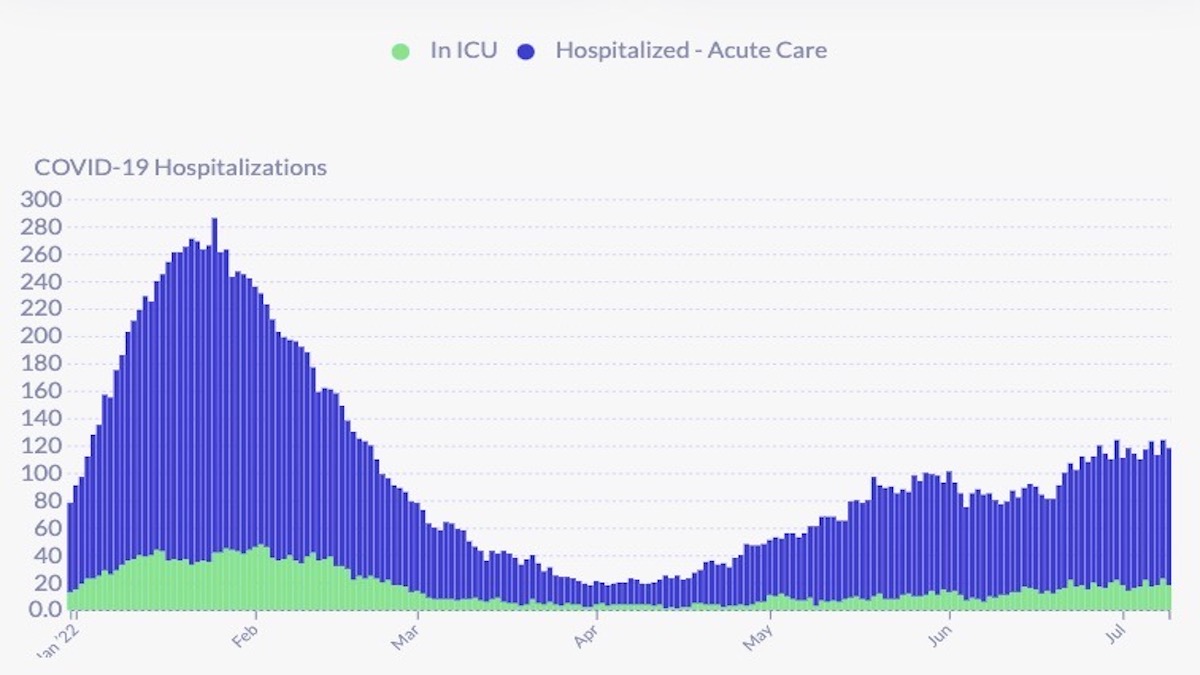
Over the past week, hospitalizations remain flat although there were ups and down during the week. On July 9, DPH reports there were 118 covid hospitalizations, or about 13.5 covid hospitalizations per 100,000 residents (based on an 874,000 population). ICU patients had climbed to 23, but have fallen back to 18. The California Department of Public Health reports 128 covid patients in SF hospitals with 23 patients in ICU as of July 12.
The latest report from the federal Department of Health and Human Services shows Zuckerberg San Francisco General Hospital with 22 covid patients and 10 ICU beds available, while across the Mission, CPMC had 11 covid patients and 5 ICU beds available. Of 130 reported covid patients in the City, 58 were at either SFGH or UCSF, with at least 86 ICU beds available among reporting hospitals (which does not include the Veterans Administration or Laguna Honda). The California DPH reports that as of July 12, SF had 105 ICU beds available. Whether those beds are actually “staffed” neither the City nor the State will say.
Between May 8 and July 7, DPH recorded 1,511 new infections among Mission residents (an increase of 3.8 percent from last week) or 257 new infections per 10,000 residents. During that period, Mission Bay continued with the highest rate at 426 new infections per 10,000 residents. Mission Bay and Bayview Hunters Point were the only neighborhoods with a rate above 400, 17 others had rates above 300 per 10,000 residents, with 11 in the east and southeast sectors of the City.
DPH reports on July 5, the 7-day average of daily new infections recorded in the City dropped to 399 or approximately 45.6 new infections per 100,000 residents (based on an 874,000 population), an decrease of approximately 9.1 percent. According to DPH, the 7-day average infection rate among vaccinated residents was 41.7 per 100,000 “fully vaccinated” residents and 110.8 per 100,000 unvaccinated residents. It is unclear whether “fully vaccinated” means 2, 3 or 4 doses. According to the New York Times, the 7-day average number on July 5 was 501. The latest report from the Times says the 7-day average on July 12 was 458, an 7 percent decrease over the past two weeks. As noted above, wastewater monitoring shows a decrease in the southeast sewers. This report comes from the Stanford model. The state says its reports are delayed due to “supply chain” issues, but early this month shows covid increasing in the sewers.
Cumulatively, the recorded infection rate for Pacific Islanders (based on group population) is 4,884 per 10,000 residents, Latinxs 2,712, Native Americans 2,356, Blacks 2,083, Asians 1,244 and Whites have a recorded infection rate of 1,109 infections per 10,000 residents.
Positivity rates continue to climb. On July 5, the 7-day rolling Citywide average positivity rate rose 5.8 percent during the past week to 16.3 percent, while average daily testing dropped approximately 15 percent. Over the past two months, the Mission has had a positivity rate of 12.3 percent. During that period, Portola had the highest rate at 16.5 percent while Noe Valley had the lowest rate at 9.6 percent (the only neighborhood below 10 percent).
Vaccination rates in SF show virtually no change from last week. 90 percent of all San Franciscans have received one shot, 84 percent two shots and 74 percent have received at least one booster. DPH estimates 80 percent of Asians have received at least one booster, 79 percent of Whites, 64 percent of Blacks, 61 percent of Latinxs, 61 percentof Native Americans and 59 percent of Pacific Islanders have received at least one booster.
For information on where to get vaccinated in and around the Mission, visit our Vaccination Page.
Eleven new covid-related deaths have been reported (none yet in July), bringing the total since the beginning of the year to 231. DPH won’t say how many were vaccinated. Nor does it provide information on the race, ethnicity or socio-economic status of those who have recently died. According to DPH “COVID-19 deaths are suspected to be associated with COVID-19. This means COVID-19 is listed as a cause of death or significant condition on the death certificate.” Using a phrase like “suspected to be associated with” indicates the difficulty in determining a covid death. The fog gets denser as DPH reports, as it has for months, only 21 of the deaths are known to have had no underlying conditions, or comorbidities. DPH only supplies cumulative demographic numbers on deaths.
The lack of reliable infection number data makes R Number estimates very uncertain. Covid R Estimation on July 8 estimated the San Francisco R Number at 1.2 while its estimate for the California R Number on July 11 was 1.27. The ensemble, as of July 10, estimated the San Francisco R Number at .93 and its California R Number at .94. Note: Four of six models in the ensemble are below 1.
In June, females accounted for 51.3 percent of recorded infection, Males 47 percent while Trans Females and Trans Males accounted for .1 percent and “Other” accounted for .9 percent.
DPH reports in June, those San Franciscans “experiencing homelessness” recorded 190 infections, or 1.4 percent of the City’s total.


Miriam, do those things until when? When will we know it’s over? Seems there’s always another reason to be scared and change our lives. When do we know that these things actually worked and our lives can now be free of fear? What is the exit strategy?
Thanks for answering my question the last time you reported and confirmed that the hospitalization numbers do not distinguish between “for” and “with” COVID. It looks like the death numbers have a higher standard than just a positive test. I am wondering now about 2 things: 1. Is there any goal or end that anyone has articulated by health authorities for what they are trying to achieve? and 2. How, exactly, am I or other readers supposed to make sense or make any decisions based on all of these charts and graphs? I am not trying to take away your gig or anything! I am just seeing everyone making their own decisions on what to do based on whatever and you see some vax requirements here and there, some masking in some places but not others, etc. I don’t get the feeling that everyone is looking at the same graphs, charts or that there is very much agreement on which ones are useful. Is it just me?
It’s not just you, Kid. It’s extremely difficult to make these calculations. These are calculations that really need to be made by our leaders and translated into policy. The Department of Public Health is pushing this “personal responsibility” narrative instead of taking any actions themselves to protect San Franciscans from mass infection. It conveniently lets them off the hook, and it’s putting us all at risk.
The key things to know right now are that transmission levels are sky-high in SF, and our mayor and SF DPH is letting it rip through the city in a way that is criminally negligent. Take all the individual protections you can, like masking, boosting, and avoiding crowds.
But we need policy, too. It’s unacceptable for our government to abandon public health and kick all this over to individuals. Especially when there’s this much virus circulating. We need to pressure our elected officials and DPH to make them to take action, like re-implement indoor mask mandates, to slow this rampant transmission. Otherwise, it’s going to result in a lot more disease and death.
We need more messaging like this, too:
https://m.youtube.com/watch?v=kX9t8jQ9-fM
Instead, we’re encouraged to accept mass disease, disability, and 1,250,000+ deaths in the U.S. — and about one a day in SF right now — as “normal.” There’s nothing normal about mass death and disability. It’s like we’re living in the 1860s. We have to fight back.