Good morning, Mission, and welcome to Virus Village, your (somewhat regular) Covid-19 data dump.
Hospitalizations, positivity rates, R Number models and wastewater monitoring are all up, while recorded infections remain flat.
Omicron sub-variants BA.4 and BA.5 are now taking over as the dominant strains in the world, and will soon be dominant in the U.S. These variants are the most contagious yet. The virulence is open to question, but a rise in hospitalizations around the world, particularly in heavily vaxxed Portugal, is not a good sign.
Here is a summary of the new variants.
What steps is San Francisco’s Department of Public Health taking to mitigate transmission or warn of the dangers posed by the new variants?
Yesterday, a subcommittee of the U.S. Food and Drug Administration recommended another booster for the fall that has been reconfigured to take into account omicron. But it was designed for omicron .1, not omicron .4 or .5. The data on the effectiveness of the vaccine is very limited, giving rise to a variety of interpretations.
Here are pros and cons for the new booster.
A “universal coronavirus vaccine” is now being tested. This seems better than chasing after variants that keep changing.
High community spread undermines the effectiveness of individual responsibility and the use limited clinical tools. Understanding the infectiousness of the airborne virus would seem logical, as would an emphasis on ventilation.
How long does the airborne virus remain infectious, and under what kind of conditions? As this article argues, understanding the impact that airborne transport has on pathogens, and the influence of environmental conditions on pathogen survival, can inform the implementation of strategies to mitigate the spread of diseases such as covid.
High community spread and re-infection increase the likelihood of long covid, says the World Health Organization. Here’s an interview with University of California, San Francisco’s Lekshmi Santhosh on what we know and don’t know about long covid.
What are the covid protocols in hospitals? Do they segregate covid patients from others? Do hospital workers wear N95s? Do they clean the air? How? And how often? Here is a summary on actions taken by academic hospitals around the country. There are no standards, and the diversity of practice is somewhat shocking. But not surprising.
What’s happening in San Francisco hospitals? Who knows? Our local celebrity experts prefer to discuss individual risk calculation, rather than what their hospitals are doing to protect workers and patients.
Determined inaction by government officials at all levels has left us vulnerable to new variants and repeated surges. But why would anyone deliberately degrade community hubs, one of the most effective and hopeful programs developed in the City? Ask Mayor London Breed. Ask Grant Colfax. As Ed Yong points out, community work has been foundational in fighting any pandemic.
Over 4 million (!!!) papers, studies and preprints have come out on covid, and we still know so little.
Scroll down for today’s covid numbers.
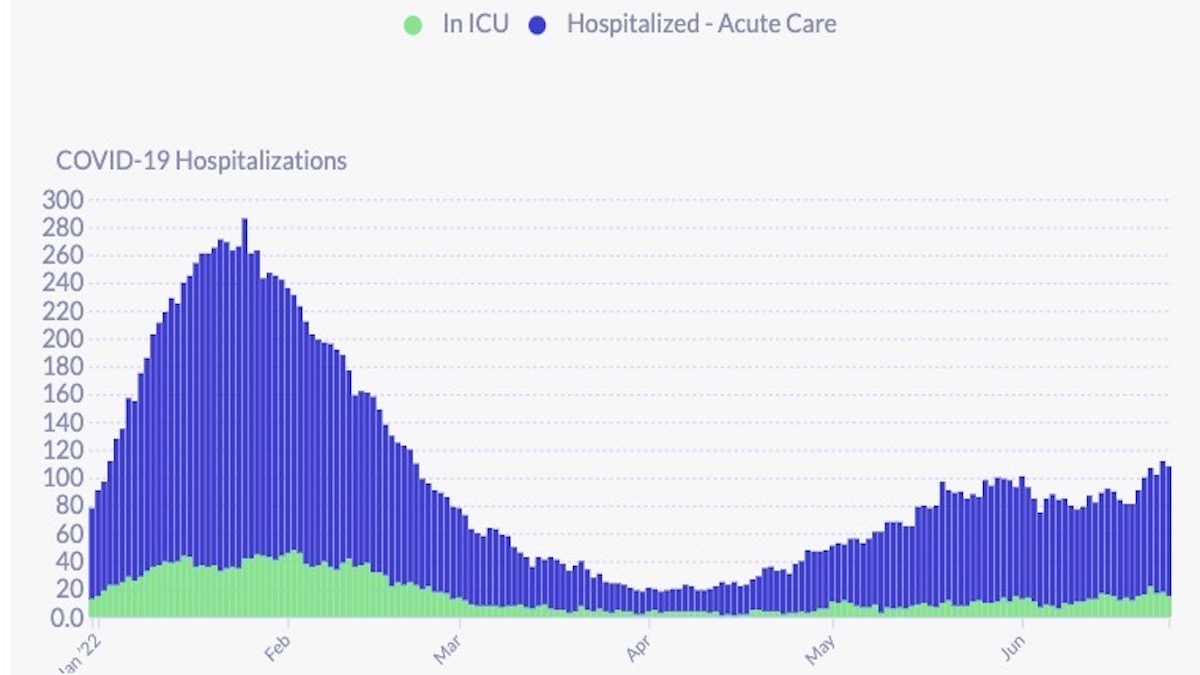
Over the past week, hospitalizations jumped 33 percent (representing 27 more patients). On June 25, DPH reports there were 108 covid hospitalizations, or about 12.4 covid hospitalizations per 100,000 residents (based on an 874,000 population). ICU patients had climbed to 22, but have fallen back to 15. The California Department of Public Health currently reports 115 covid patients in SF hospitals with 23 patients in ICU.
The latest report from the federal Department of Health and Human Services shows Zuckerberg San Francisco General Hospital with 12 covid patients and 8 ICU beds available, while across the Mission, CPMC had 8 covid patients and 4 ICU beds available. Of 106 reported covid patients in the City, 52 were at either SFGH or UCSF, with at least 72 ICU beds available among reporting hospitals (which does not include the Veterans Administration or Laguna Honda). The California DPH currently reports 104 ICU beds available in San Francisco.
Between April 25 and June 24, DPH recorded 1,389 new infections among Mission residents (an increase of 5.8 percent from last week) or 250 new infections per 10,000 residents. During that period, Mission Bay continued with the highest rate at 432 new infections per 10,000 residents. Although Mission Bay was the only neighborhood with a rate above 400, 14 others had rates above 300 per 10,000 residents, with 9 in the east and southeast sectors of the City. In a surprise, Seacliff posted a rate of 327 per 100,000 residents (perhaps the City will pay more attention to transmission now).
DPH reports on June 21, the 7-day average of daily new infections recorded in the City rose to 422 or approximately 45.7 new infections per 100,000 residents (based on an 874,000 population), basically flat since last week. According to DPH, the 7-day average infection rate among vaccinated residents was 48.2 per 100,000 “fully vaccinated” residents and 94.8 per 100,000 unvaccinated residents. It is unclear whether “fully vaccinated” means 2, 3 or 4 doses. According to the New York Times, the 7-day average number on June 21 was 465. The latest report from the Times says the 7-day average on June 28 was 492, a 1 percent decrease over the past two weeks. As noted above, wastewater monitoring shows a substantial rise in the southeast sewers. This report comes from the Stanford model. The state is still reporting “staffing problems.”
So far in June, Asians recorded 3,279 new infections or 31.1 percent of the month’s cases; Whites 2,388 infections or 22.6 percent; Latinxs 1,333 infections or 12.6 percent; Blacks 484 infections or 4.6 percent; Multi-racials 72 infections or 0.7 percent; Pacific Islanders 54 infections or 0.5 percent; and Native Americans had 23 recorded infections in May or 0.2 percent of the June totals so far.
On June 21, the 7-day rolling Citywide average positivity rate rose 10.9 percent during the past week to 14.3 percent, while average daily testing dropped approximately 7.4 percent. Over the past two months, the Mission has had a positivity rate of 10.8 percent.
Vaccination rates in SF show virtually no change from last week.
For information on where to get vaccinated in and around the Mission, visit our Vaccination Page.
Nine new covid-related deaths, with 7 more in June, have been reported, bringing the total since the beginning of the year to 215. DPH won’t say how many were vaccinated. Nor does it provide information on the race, ethnicity or socio-economic status of those who have recently died. According to DPH “COVID-19 deaths are suspected to be associated with COVID-19. This means COVID-19 is listed as a cause of death or significant condition on the death certificate.” Using a phrase like “suspected to be associated with” indicates the difficulty in determining a covid death. The fog gets denser as DPH reports, incredibly as it has for months, only 21 of the deaths are known to have had no underlying conditions, or comorbidities. DPH only supplies cumulative demographic numbers on deaths.
The lack of reliable infection number data makes R Number estimates very uncertain. Covid R Estimation on June 24 estimated the San Francisco R Number at 1.21 while its estimate for the California R Number on June 27 was 1.26. The ensemble, as of June 26, estimated the San Francisco R Number at .97 and its California R Number at .97. Note: All but one model in the ensemble show SF under 1.
So far in June, DPH reports 56 new infections and 0 new deaths in nursing homes (“skilled nursing facilities”), while in SROs (“Single Room Occupancy hotels”), DPH reports 40 new infections and 1 new death.


By the way, BART still requires masks, but apparently they might be reconsidering that decision sometime soon, even as we’re in the middle of a surge. If you’d like to leave them a comment saying that you support masking on public transit and why that’s important to you, you can do so here: https://www.bart.gov/contact/comments
“Require” has been a pretty loose term since they first dropped the actual requirement months back. Yeah, they re-instated it soon after, but the damage was already done: people had already begun not wearing them and the dropped requirement (re-instated or not) just left us with a 50/50 (at best) average for what we see everyday.
I know I’ll still wear both of mine along with my face shield, but I wouldn’t be surprised if I’m the only one.
Mask mandates aren’t perfect, true. But multiple studies have shown that they make a difference, and the people are more inclined to wear masks when mandate is in place. Even if it’s not being enforced and people aren’t complying perfectly, it definitely makes a difference to have one in place. And BART should keep theirs.
I’m not objecting to mask mandates – quite the contrary, they never should have been dropped in the first place. Hell, I’ve pontificated on them ad nauseum: https://48hills.org/2022/05/unlike-london-breed-i-never-took-my-mask-off-now-covid-cases-are-up-again/ What I’m saying is that BART dropping their mask mandate (albeit briefly) opened the floodgates to all the non-maskers infecting the system now. And since there aren’t any mandates outside of BART – city-wide or otherwise – the transit has no way to enforce theirs in any way, putting all of us in danger.
Now, we have to ride with heavy mouth-breathers because Breed and others took the shitty “advice” of anti-maskers like Monica Gandhi.
Good point. And that’s a great article. Agreed, it would have been far better for BART to have not dropped the mandate in the first place. But I still think it’s very worthwhile to fight to keep it from being dropped again, especially considering how sky-high the numbers are in the Bay Area right now. Dropping it would only make things worse.
If anyone else wants to contact BART to urge them to keep the mask mandate, I’ve heard it’s better to e-mail them than to use the comment link:
Rebecca.Saltzman@bart.gov (BART Board president)
boardofdirectors@bart.gov (sends an e-mail to each of them)
Why do you still rely on SFDPH case numbers? The New York Times reports as of June 28 the weekly average in SF is 564 cases/day. And yes, this is mass murder by another name: the current daily average of deaths in the US due to Covid is 338. In one month that’s 11,640 PREVENTABLE deaths. New research shows that *25%* of children infected with Covid get Long Covid (study here: http://www.nature.com/articles/s41598-022-13495-5)
Why is this allowed to happen? Aggressive testing, free vaccines, masking, and HEPA indoor ventilation work. It’s not that difficult or expensive. Why are Democratic politicians caving to the anti-vax, anti-mask crowd? (I know: $$$). I’m beyond outraged at how depraved they are.
This is a lot more informative than another one of Monica Gandhi’s bullshit “COVID is over” op-eds in The Chronicle. I’d also recommend Violet Blue weekly Pandemic Round-Ups every Thursday (free on Patreon): https://www.patreon.com/VioletBlue/posts
Seriously, with COVID still killing people and monkeypox riding around the edges, this is not the time to stop boosting, masking, or social distancing.
Thanks for pointing us to Violet Blue’s Pandemic Round-Up, Charles. I hadn’t read that before. Wow, tons of excellent information.
It’s been the single most-accurate aggregation of COVID info for the past 2 1/2 years.
You need to pick a metric- some of your numbers are cases per 10K and some are per 100K. For clarity’s sake, please pick a system of measurement and stick with it! It’s impossible to tell if it’s a typo or on purpose when you use both in the same paragraph.
Thanks again for the great work, Mark.
“Mission Local will follow up with more reports on the disabled and immunocompromised,” this column proclaimed weeks ago. But I haven’t seen anything yet on that front. Mission Local: please come through on this. There are so many great people you could talk to.
I’d love to hear how medically vulnerable San Franciscans are navigating this pandemic, especially as San Francisco has embraced an inhumane, eugenicist “let it rip” strategy, getting rid of all mitigation measures.
Harsh words? Not really. Who’s likeliest to die from a “let it rip” strategy? The medically vulnerable. So what does that boil down to, really? Eugenics.
How can we not care about this?
Make no mistake, this is going to affect more and more able-bodied people, too, as more people develop Long Covid. It’s not going to be pretty when B5 rips its way through the Bay Area, especially if SF DPH won’t even bring back the most basic of mitigations, such as mask mandates on public transit.
The medically vulnerable aren’t given many options here, and it’s unacceptable. They’re expected to stay home forever, or risk terrible outcomes in order to do essential things such as grocery shopping or going to a medical appointment.
I urge you to do just one piece that examines this huge problem that’s getting virtually no local coverage.