Good morning, Mission, and welcome to Virus Village, your (somewhat regular) Covid-19 data dump.
Hospitalizations are plateauing, while positivity rates and recorded infections continue trending downward. Recent R Number models show San Francisco below 1.
Some consider San Francisco’s relatively low covid numbers to be, among other factors, a consequence of what the City learned from the HIV/AIDS crisis in the ’80s and ’90s. Many still remember the struggle to get San Francisco’s Department of Public Health to pay attention to the disease and to respond with more than closing bathhouses. Although some doctors, like Diane Havlir, put their experience with HIV to valuable use in confronting covid, DPH has displayed little institutional memory. Reading this essay reminded me of those battles, and pointed to similarities in the covid crisis, especially at this stage.
HIV and covid have a more tangled, and perhaps more intimate, relationship. Omicron may owe its origin to the HIV pandemic in southern Africa, which continues to be a common cause of immunodeficiency in a region where HIV activists have played a key role in local public health responses to covid.
At a conference on retroviruses and opportunistic infections, Scottish epidemiologist Muge Cevik reviewed covid’s global epidemiology and concluded that “people are not the drivers of transmission, it’s their unmet needs; we need a systems approach in pandemic response & evidence synthesis is crucial for policymaking.”
The first lesson to learn from the HIV pandemic is “a need to anticipate health inequalities. Pandemic HIV transmission accelerated among mobile, well-connected networks, but the burden shifted to poorer people and countries, young women, and marginalized groups.”
Two recent studies, here and here, show covid’s unequal toll on “essential(ly) screwed” workers, which should, by now, come as a surprise to no one. Given DPH’s slow, stumbling effort to respond to San Francisco’s health inequalities, which have been in the forefront again during omicron, it’s fair to ask what DPH has learned, and what systems are being put in place to not only protect hospitals from getting overwhelmed, but to enhance the health of everyone in the City.
Although I haven’t read the details, from what I’ve seen, California’s “endemic’ policy does not address inequities, even though Latinx residents generally, and farm workers in particular, have been the most affected by the virus over the past two years. Newsom’s photo op also did not address single-payer health insurance, a major campaign promise in 2018.
Mask mandates have been lifted, and the masked scene at the Chase Center, where over 15,000 gathered Wednesday night, was decidedly mixed. Although the Dubs’ dismal defeat should not be blamed on the lack of masks, concession workers fear a greater loss may be looming.
Should those unvaxxed who have been infected by the virus be banned by vaccine mandates? Multiple studies show prior covid infection can provide equivalent or better protection than from vaccination. The Centers for Disease Control and Prevention recommends a three-shot regimen for all Americans 12 and older, regardless of whether they have had a previous infection. Some still consider this not only overkill, but a waste of vaccine.
Although early studies indicated children could suffer symptoms associated with Long Covid, several recent “peer-reviewed ” (emphasis added!!!) studies suggest that Long Covid in children is rare and, when it does occur, is short-lived.
Finally, to end on a down note, we knew the pandemic forced many short-staffed hospitals to rely on “traveling nurses.” But did you know that private equity firms bought up travel nurse staffing agencies and profited handsomely? If you want to learn more, but don’t want to sign up for STAT+, check out this letter from the American Hospital Association and American Health Care Association.
Scroll down for today’s covid numbers.
As of Feb. 17, DPH reports 782,560 residents have been vaccinated, more than 89 percent of all San Francisco residents have received one dose, and over 83 percent have received two. For residents 5 and older, DPH reports the figures rise above 90 percent and above 86 percent while for those 65 and older over 90 percent have received two doses. SFDPH reports that as of Feb. 17, approximately 467,159 SF residents (65 percent of all residents, 82 percent of residents 65 and older) have received a COVID-19 booster dose.
For information on where to get vaccinated in and around the Mission, visit our Vaccination Page.
On Feb. 12, DPH reports there were 161 covid hospitalizations, or about 18.4 covid hospitalizations per 100,000 residents (based on an 874,000 population). ICU patients have been plateaued since Feb. 4. Today, the California Department of Public Health reports 153 covid patients in SF hospitals and 33 ICU patients. Unlike it’s counterparts in New York, Seattle — even Los Angeles — DPH cannot report how many covid patients are vaxxed and how many unvaxxed since September 1. Nor does DPH provide any demographic data whatsoever making it impossible to know the degree to which populations and neighborhoods have been affected.
The latest report from the federal Department of Health and Human Services shows Zuckerberg San Francisco General Hospital with 25 covid patients and 6 ICU beds available, while across the Mission, CPMC had 20 covid patients and 2 ICU beds available. Of 225 reported covid patients, 96 were at either SFGH or UCSF, with at least 67 ICU beds available among reporting hospitals (which does not include the Veterans Administration). The California DPH currently reports 75 ICU beds available in San Francisco. Note: The Government Accountability Office (GAO) has issued a scathing report for sustained public health crisis failures at HHS. The failures cited include “collecting and analyzing data to inform decisionmaking.”
Omicron revived SF’s standard pandemic pattern, hitting the lower socioeconomic sectors of the City the hardest. Between Dec. 15 and Feb. 13, DPH recorded 4429 new infections among Mission residents or 754 new infections per 10,000 residents. Bayview Hunters Point had the highest number of recorded new infections (4606) with a rate of 1215 new infections per 10,000 residents. Of 38 neighborhoods, 14 had rates above 700 per 10,000 residents, 13 in the east and southeast sectors of the City. Seacliff had the lowest rate with 383 new infections per 10,000 residents and Lakeshore, the only neighborhood in the City with a vaccination rate below 50 percent, had the second-lowest rate at 434 new infections per 10,000 residents.
DPH reports on Feb. 10, the 7-day average of daily new infections recorded in the City dropped to 299 (under 300 for the first time since Dec. 19) or approximately 34.2 new infections per day per 100,000 residents (based on an 874,000 population). According to DPH, the 7-day average infection rate among vaccinated residents was 30.2 per 100,000 “fully vaccinated” residents and 76.4 per 100,000 unvaccinated residents. It is unclear whether “fully vaccinated” includes boosters or the infection rate among those vaccinated with 2 doses.
In January, DPH reports Asians had 25.5 percent of the month’s total, up from 19.7 percent in December; Latinxs had 21.6 percent, up from 18.4 percent, Whites had 20 percent, down from 33.4 percent; Blacks 5.8 percent, up from 4.7 percent, Multi-racials had 1 percent, down from 1.2 percent, Pacific Islanders had 1 percent, the same, and Native Americans had .2 percent of January’s total, down from .3 percent in December.
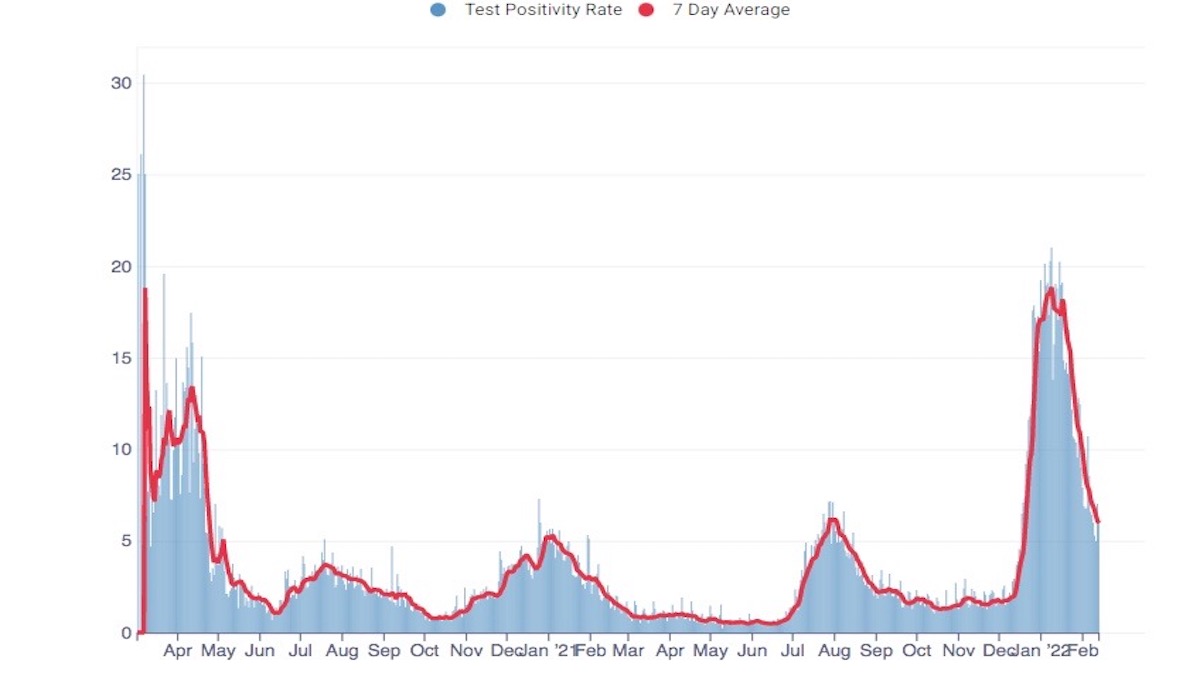
On Feb. 10, the Citywide 7-day average positivity rate dropped below 7 percent for the first time since dec. 21. In January, DPH reports San Francisco’s Latinx residents had a positivity rate of 22.4 percent, up from 10.7 percent in December; Pacific Islanders 22.1 percent, up from 12 percent; Blacks 20.2 percent, up from 9.2 percent; Multi-racials 17.9 percent, up from 9.2 percent; Native American 17.8 percent, up from 10.2 percent; Asians 14 percent, up from 6.6 percent; and White San Franciscans had a January positivity rate of 12 percent, up from 8.4 percent in December.
There have been 68 covid-related deaths since the beginning of the year. Probably most are related to omicron. DPH won’t say how many were vaxxed and how many unvaxxed. Nor does it provide information on the race/ethnicity or socio-economic status of those who have recently died. According to DPH “COVID-19 deaths are suspected to be associated with COVID-19. This means COVID-19 is listed as a cause of death or significant condition on the death certificate.” Using a phrase like “suspected to be associated with” indicates the difficulty in determining a covid death. The ambiguity is heightened when currently it is unknown whether or not 34.5 percent of the deaths had one or more underlying conditions. As of Feb. 9, DPH continues to report only 21 of the 761 deaths are known to have had no underlying conditions, or comorbidities.
Covid R Estimation has not updated its San Francisco R Number since Feb. 8. It is still at 1.07. On Feb. 16, it estimates the California R Number at .49. The ensemble lowered its average San Francisco R Number to .81 and its average California R Number to .55. Of all models currrently reporting in the ensemble, the SF R Number ranges from .63 to .96.
During the course of the pandemic, San Franciscans aged 0-20 had 0 covid-related deaths, or 0 percent of the total; 21-29 3 deaths, or .4 percent; 30-39 12 deaths, or 1.6 percent; 40-49 29 deaths, or 3.8 percent; 50-59 54 deaths or 7.1 percent; 60-69 113 deaths or 14.8 percent; 70-79 141 deaths or 18.5 percent; and those San Franciscans 80 and older suffered 409 deaths or 53.7 percent of all San Franciscan covid-related deaths, even though they had just 2.3 percent of the City’s recorded infections.


Why don’t you address the very high death rate in SF? As of yesterday, according to the New York Times, the death rate has climbed 260% over the past two weeks. The number of deaths in February is the highest of any month in the pandemic. This needs to have a spotlight put on it.
“DPH reports on Feb. 10, the 7-day average of daily new infections recorded in the City dropped to 299 (under 300 for the first time since Dec. 19)”
This is also the first time the [post-peak] 7-day average of daily new infections from Omicron has fallen below the Delta peak (310 on Aug 2). That’s something.