For all the talk of equitable vaccine distribution and celebration of essential workers, Black and Latinx groups, as well as low-income or otherwise vulnerable groups, have largely been left behind in California, particularly in areas of the state where they bore the brunt of the virus.
The exception is San Francisco, where heavily impacted areas have seen massive community-led efforts to test and vaccinate. And while these have succeeded in the Latinx population, where 76 percent of eligible Latinx residents are vaccinated, they have failed to do as well in the Black population, with only about 60 percent of eligible Black residents vaccinated.
But, in other parts of the state, where Latinx and Black residents also saw high rates of infections and deaths, vaccination rates are below 50 percent. In many cases, way below.
Kings County, for example, reported one of the highest infection rates in the state: More than 23,000 cases and 247 deaths in a population barely over 150,000. Meanwhile, of the most vulnerable quarter of the county’s population, only 33 percent are now vaccinated. That quartile includes residents most likely to be infected, or with less access to healthcare.

Only about a quarter of the “least healthy” population has been fully vaccinated in Kings County. 
Less than 20 percent of the Black population has received a vaccine dose.
In nearby Merced County, also located in the Central Valley, there have been similarly high infection rates, and less than half of that same vulnerable quarter of the population has been inoculated.

Only 35 percent of the “least healthy” population has been fully vaccinated in Merced County. 
Only about 25 percent of the Black population has received a vaccine dose.
These numbers are not unique to the Central Valley: Up in Del Norte County, only 35 percent of the lowest quartile is vaccinated, albeit in a much smaller population. A jarring 93 percent of Black residents and 81 percent of Latinx residents are unvaccinated.
Down south in Imperial County, which shares a border with Mexico, almost 88 percent of the Black population remains unvaccinated. And the issue is not an exclusively rural one: Even Los Angeles County reports almost 57 percent of Black residents and 53 percent of Latinx residents as unvaccinated – that’s over 2.5 million people.
By contrast, of the 32,000 plus residents in San Francisco’s lowest health quartiles, 80 percent have been vaccinated.
Infectious disease specialists and epidemiologists say low vaccination rates elsewhere indicate barriers to access, which can take many forms. UCSF epidemiologist Dr. Kirsten Bibbins-Domingo points to reliable transportation or proximity to vaccine sites, language or digital barriers, and sometimes just a simple lack of information in the communities that most need the vaccines.
Transportation
A Vaccine Equity Planner launched June 9 by Ariadne Labs and Boston Children’s Hospital shows “vaccine deserts” across California, where access to a shot takes more than 30 minutes by public transit or more than 15 minutes by car.
These areas span most of the state outside of larger cities: the Central Valley and rural northern and southern California, including Imperial County, the hardest hit in the state. When you compare the vaccine desert locations to the areas ranking lowest in the Centers for Disease Control’s social vulnerability index, there’s nearly a full overlap.
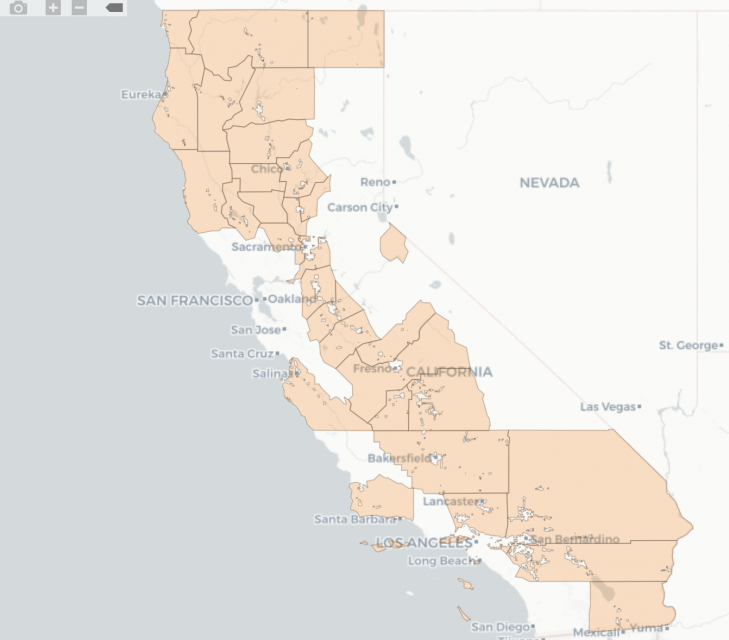
Highlighted in orange are “vaccine deserts,” defined as places where it’s more than 30 minutes by public transit to the closest active COVID-19 vaccination site, in areas with high social vulnerability. 
CDC Social Vulnerability Index data for 2018, with most vulnerable counties shown as dark blue.
When vaccines first became available, researchers like Bibbins-Domingo and Dr. Diane Havlir, the leader of the Unidos en Salud campaigns in the Mission District, recommended vaccine distribution prioritize the most impacted zip codes to ensure equity. Instead, the state decided to focus vaccination efforts on getting vaccines into arms of the most vulnerable by age, regardless of socioeconomic status or exposure risk.
But getting to mass vaccination sites at expo centers or sports arenas often required having a vehicle and time off work to wait in long lines.
To capture residents without such luxuries, the Bay Area quickly added a layer of pop-up and local sites. Moreover, the early community work by UCSF doctors, the Latino Task Force and other community groups, helped to engender trust.
The latter, said researchers, can be the key to overcoming vaccine hesitancy.
Trust
“If they’re not rushing out to get vaccines on the first day, they generally want to get information from people they trust,” Bibbins-Domingo said.
This doesn’t mean these individuals wouldn’t want to be vaccinated at all, but that they’d be more receptive to getting the vaccine from their primary care doctor or members of their community who know them and speak their language, literally or figuratively.
In part, San Francisco’s success in reaching more vulnerable populations has been enabled by early and intense outreach by local community groups testing in the communities.
It took a lot of work.
Dr. Carina Marquez, an infectious disease fellow at UCSF, said outreach with the Latino Task Force included door-to-door sign ups that don’t require computer literacy, social network mobilization through Latino-focused organizations, and even word of mouth referrals through community ambassadors.
These days, the Unidos En Salud vaccine site – an alliance with the Latino Task Force, UCSF and the SF Department of Public Health – has bilingual, usually Latino doctors stationed at the corner of 24th and Capp for “Cafecitos,” where people can stop in on their way through the neighborhood. “We have some pan dulce and coffee and people passing by just ask their questions of the doctor,” said Marquez.
Cafecitos are intended to help inform those with questions or still on the fence about getting vaccinated, in a comfortable home setting.
Different strategies have been employed for Black communities, which were historically exploited in the name of science and are also more dispersed in the Bay Area, said Dr. Kim Rhoads, an epidemiologist and bio-statistician at UCSF.
“Immigrants get to kind of choose where they live. But Black people didn’t get to choose. Black people get displaced,” said Rhoads, one of the leaders of Umoja Health, a community, UCSF and county effort in Alameda county. “You can’t just be in one place and service the African American community across the county, or even across the city for that matter.”
The Umoja pop-ups went to places where Rhoads said the public health department and the county clinics would never go, places like the liquor store and the local bar.
At this point, it’s up to the state and county officials to partner with community groups and leaders to figure out what works for them, Bibbins-Domingo said, and different places will have success with different solutions. And adapting to unique situations is necessary, especially as circumstances change, like the demand for vaccines.
“We have to think in a little bit more creative ways, and that likely will have to be adapted to each county,” Bibbins-Domingo said. But this doesn’t mean the community organizers or even the counties alone are responsible. The state plays a large role in the inequities we see now, looking back.
“I do think that the delay in adopting more local strategies is, in part, why we’ve not vaccinated to a higher rate,” she continued, indicating that many warned early on that mass vaccinations or distribution to pharmacy chains like Walgreens alone would never be sufficient to get all groups vaccinated.
Why the state hasn’t done more in the counties that suffered most is unclear.


Why is no one talking about the negative social control at the community level? We hear the community leaders, the activists, the preachers, again and again insisting on keeping alive ideas about the healthcare system being against their people. In the time of covid, these OUTDATED lies about the outside world only serves the community leader in keeping control over people. Covid revealed the reality many vulnerable people across the US face – they don’t have any true advocates, only people who got wealthy by exploiting and deepening the misery of their own people! Is anyone holding community leaders accountable for the results of spreading self-destructive lies and conspiracy theories? Is anyone scrutinizing social control in minority groups? People falling ill or dying during a pandemic is the ultimate consequence of these outdated power structures. When we refuse to hold these local power structures accountable we are enabling them.
LatinX? Latino’s don’t use that term. Stop with the nonsense PC terms.
I live in Merced and the biggest problem was the unfair distribution of vaccines. Our area got only a third of the number of vaccines per capita than the more populated cities, including Los Angeles. Yet, we have one of the biggest populations of essential food production workers – mostly low income and many Latinos. I suspect other undervaccinated counties experienced the same withholding of vaccinations early on. Governor Newsom is unfair to the Central Valley population in many other ways too, including extraction of our fresh water supplies that impact clean drinking water to many of our rural communities. The City of Merced relies 100 percent on groundwater for drinking water so the ability to use surface water for recharge is essential. But vaccinations should have been sent fairly by poplulation counts to ALL parts of the state.
why the state hasn’t done more in the counties that suffered most is very clear when you look at what has happened, and keeps happening. this is the “new normal”, same as the “old normal”
I’m confused. How do those numbers tell me anything about equity when they’re not compared to other populations? For example, you note that in Kings County “of the most vulnerable quarter of the county’s population, only 33 percent are now vaccinated.” That’s a low number, but it says nothing about equity without comparing it to other numbers. Could you add some more data to show how equity is relevant?
I just don’t think this is an equity issue. There is plenty of access to free vaccines all over the state – even in the poorest, most remote sections of California. Free, same day vaccinations are available at CVSs and Walgreens all over the counties mentioned in the article. (I checked.) Also, every county health department has free vaccines waiting – no appointment necessary.
Isn’t it embarrassing enough that the state has to give away hundreds of millions of dollars on a vaccine lottery just to entice people to get a free shot that may save their life?
I just think there is a large portion of California that is willfully ignorant, or lazy, or both.
It could be an equity issue, the points you raised aside. There are many reasons why certain populations could still end up with lower vaccination rates – access to information, historical distrust of govt., etc. However, this article does NOTHING to demonstrate that. Simply throwing out low numbers among certain populations and stating the issue is equity is at best lazy and at worst a lie. Show us with the numbers. Throw the vaccination rates of other populations on those counties or overall vaccination rates in those counties for comparison. Or change the title.