With 12 days until a highly contentious election, a third wave of the coronavirus pandemic is appearing in various stages across the United States — California is a notable exception, at least so far—said Dr. Bob Wachter, UCSF Grand Rounds moderator and chair of the university’s Department of Medicine.
Through on-the-ground updates from the Bay Area to Wisconsin to South America, this week’s panel made it clear that Covid-19 is not disappearing anytime soon, even as vaccine development moves at “warp speed.” As both individuals and policy makers continue to balance the desire to live our lives with our tolerance for risk, Wachter also brought in a speaker to discuss decision-making and risk management during this indefinite pandemic.
Case count and death rate updates
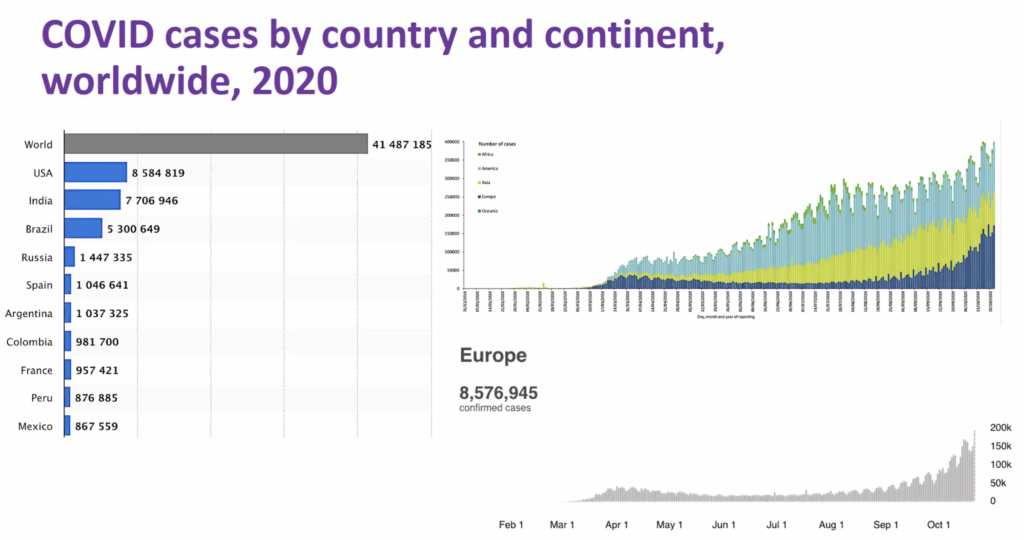
UCSF professor of epidemiology Dr. George Rutherford opened the session with overviews of local and worldwide covid statistics. The United States currently leads in case counts with 8.4 million cases. India is trailing by about 800,000 cases. Four of the top 10 countries with the highest number of cases are in South America, and Europe is currently experiencing a surge, with both Wales and Ireland moving to lock down their economies.

Cases in the U.S. have increased by more than 100 percent since their lowest point in September, with an average of 60,000 cases per day, Rutherford said. “The third wave is clearly here. This is no longer theoretical.”

Nationally, we have not yet seen a third wave of deaths.
California has managed to avoid a third wave so far, though Rutherford noted that we could see one in a few weeks, and felt that “we’re teetering at the precipice and we need to be absolutely, positively clear that we need to do everything we can to avoid infection.”
The state’s positivity rate is currently 2.6 percent, and hospital bed occupancy is the lowest it’s been since mid-April, he said. Rutherford believes that California is faring better than other parts of the country because of greater acceptance of protective measures, a slower reopening, contact tracing, a mature quarantine/isolation system, and control over institutional outbreaks.
In the Bay Area, cases continue to fall and the virus’s reproduction number (the number of people an infected person is likely to infect) is below one, in all counties except for Solano.
Report from the Wisconsin frontlines
Wisconsin is currently experiencing “by far the largest surge [of covid] we’ve seen in our state,” said Dr. Ann Sheehy, associate professor of medicine and chief of the division of hospital medicine at the University of Wisconsin-Madison. Describing her hospital, she said, “Our volumes are about twice our peak that we had in the spring. And our state statistics indicate that that will likely grow.” The hospital has a total of 592 beds and more than 40 patients, up from five or 10 cases a month or two ago. Though these numbers may sound low, hospitals in other counties of Wisconsin are experiencing limited hospital capacity.
Dr. Andrew Braun, assistant professor of medicine and director of the University of Wisconsin Health Adult Cystic Fibrosis Clinic, noted that in his Wisconsin county, there was an early mask mandate in the spring, and that residents typically wear masks outside. However, challenges to public health mandates in the courts hindered efforts to send out consistent messages, Sheehy said.
Most recently, the statewide mask mandate and 25 percent indoor capacity rate have been challenged in court, and the stay-at-home order was overturned in May.
Since then, the situation in Wisconsin has worsened.
“We’ve obviously had this chronic broiling going on for the last six to seven months as everywhere. And so now, getting to the point where we see our surge is coming, we are really working hard to talk about resilience,” Braun said.
Sheehy described how hospital staff learned a lot from the spring to help them develop a more measured response and additional medicine teams. “None of us wanted to have experience in this field, but it has helped us overall,” she said.
Regional community hospitals at the epicenter of the outbreaks in Wisconsin’s northeast are at 100 percent capacity with reports of 20 to 30 percent of patients testing positive, Braun said, calling his hospital a “feeder system” for transfers from these saturated sites.
Some of these areas received five to six inches of snow last weekend, which is cause for concern, given the increased spread of the virus indoors.
Evaluating risks in decision-making
Dr. Julia Marcus, associate professor of population medicine at Harvard Medical School, closed out the panel by discussing the difficulties of making choices and weighing risks as the pandemic continues for an indefinite stretch of time.
Though messaging at the beginning of the pandemic was often binary (stay at home, or for those who were not privileged enough to do so, go to work), Marcus saw a need to shift to a more sustainable approach as the lockdown stretched on for months.
“We’re always trading off something and we have to figure out how to do that in a way that’s sustainable not just for individuals, but also on a societal level,” she said, discussing the complexities that arise when weighing the risk of community spread, seeing family for mental health reasons, sending children to school, and more.
We can give up many things for some amount of time, but not indefinitely, especially in a situation like the pandemic, Marcus said. There will eventually be situations where you must take some risk. When faced with a difficult decision (such as going back to work for economic purposes, or visiting a loved one who is dying), she said we should be asking, “how can I do this as safely as possible?”
“I think our messaging and our policies need to be kind of framed from that perspective of acknowledging that people cannot eliminate risk from their lives,” she said. “So we have to give people guidance on how to do things as safely as possible, just like the safer sex education.”
Marcus noticed parallels between moralistic shaming online today and the shaming that took place during the HIV/AIDS epidemic, noting that such strategies were ineffective then and have actually contributed to stigmatization and further inequities.
“Seeing that really made me want to provide a framework of what has helped guide HIV prevention toward a more humane response, which is more of a harm reduction framework, as opposed to this kind of abstinence only model that frames everything as a personal choice than a personal failure,” Marcus said, remarking that focusing on unmet needs can help us be vigilant in higher risk setting. With some pushback from Wachter, she did note that the HIV analogy isn’t perfect, as covid has a much higher chance of being “explosive” with super-spreader events.
One of the reasons it is so difficult to make so many decisions each day is a lack of support from our federal government in terms of helping people stay home, giving people safer alternatives, and giving good guidance with a national unified public health voice, Marcus said. “It’s like our parents left the room and we’re trying to figure this out on our own.”
More time to figure out these answers doesn’t seem to be helping. In fact, pandemic fatigue often makes these decisions harder, she said.
“We need to recognize, too, from a public health kind of a population perspective, that people are exhausted,” Marcus concluded. “And I think we need to give them something and give them a sense of ease in some places.”
See our previous Grand Rounds coverage here.